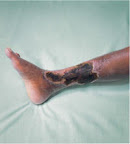
 Betty was 95. She lived in a nursing home. She was delirious and bedbound. She had diabetes, emphysema, untreatable ischaemic heart disease, and a recent stroke. And now she had a fever and a gangrenous leg.
Betty was 95. She lived in a nursing home. She was delirious and bedbound. She had diabetes, emphysema, untreatable ischaemic heart disease, and a recent stroke. And now she had a fever and a gangrenous leg.She was going to die, sooner or later.
"She's a fighter" her son said. "Before she became delirious, she told me that she'd rather lose her leg than die."
I didn't say what I was thinking - "This is not a life. You are just torturing her. She is going to die anyway."
Instead I say: "I appreciate what you are saying, but you must understand that amputating her leg has a very high chance of killing her, both immediately and in the near future. And even if she were to survive that operation her quality of life would only be worse, not better. She would definitely never walk again."
"We know that, doc, but we'd rather she die under an anaesthetic than like this. We know that's what she'd want. She doesn't walk as it is."
Perhaps I am weak, but I cannot flat out refuse to do it. I don't know for certain that she will die. She might pull through. Her chances are poor, but they are not zero.
Two days later she is awake and talking to her family. She thanks me for doing the amputation, and goes back to her nursing home. A week later I hear that she has had a "heart attack" and has passed away.
-----
Jerry is 70. He came from a hostel. He was confused but relatively independent , until he developed acute appendicitis. A diagnosis made at laparotomy. He makes a good recovery, but unfortunately, a pressure sore develops on his heel. Bone is exposed, and needs debridement. Malnutrition limits what healing is present. The arterial supply is limited. He is too confused to eat. He needs nasogastric feeding, an angiogram and a small operation to clean his ulcer."We don't think he would appreciate it, doc." said the daughter. "He doesn't know what is going on. He won't want to risk losing his leg. We're sure he wouldn't want a tube in his nose. Why can't we let him die with dignity?"
"He is not going to die anytime soon." I say. "But this ulcer will be with him for the rest of his days unless we remove the bone and put a skin graft on it. The ulcer won't kill him but it will cause him pain."
"We think he's had enough. We'd like to speak to the palliative care nurse."
Palliative care takes him over and he is dosed up to his eyeballs with subcut morphine. A month later he is still alive. I wonder how long he will last at the hospice, and how much morphine he can handle.
-----
 John was 65, living with cerebral palsy, schizophrenia, and a recently fractured humerus. Paraplegic and confused. He had recently been transferred into a nursing home where he was fully dependent. Now he had severe, sudden onset abdominal pain. There was gas under his diaphragm. There was no doubt he had a perforated viscus. Probably a duodenal ulcer. Laparotomy would be straightforward and life-saving. "I'm not going to die, doc. Just give me some pain killers and let me go home. I don't want an operation." he said.
John was 65, living with cerebral palsy, schizophrenia, and a recently fractured humerus. Paraplegic and confused. He had recently been transferred into a nursing home where he was fully dependent. Now he had severe, sudden onset abdominal pain. There was gas under his diaphragm. There was no doubt he had a perforated viscus. Probably a duodenal ulcer. Laparotomy would be straightforward and life-saving. "I'm not going to die, doc. Just give me some pain killers and let me go home. I don't want an operation." he said.There was no family. They had abandoned him years ago. His sister hung up the phone when rung at 2am in the morning. The GP that normally treated John was on holiday. From the little information I could gather, his quality of life was non-existent. Who do I ask? Who do I turn to? Do I have the right to decide whether to operate or palliate? In his incapacitated state does he have the right to refuse surgery?
So I passed the buck, and called the Chief Medical Officer. "What do I do?" I ask. "You are authorised under law to do as you see fit. As the clinician on duty, the hospital will support your decision." came the drab reply over the telephone.
So I wrote up the omeprazole, turned up the morphine infusion, and went back to sleep.





2 comments:
tough cases... the icu brings so many difficult situations like this. i don't practice there, but in training it always saddened me.
The ICU patients were in a sense easier and more difficult. You knew that they were seriously unwell, and would die immediately if you withdrew organ support, but because you had the facilities to continue it, the threshold for cessation of therapy was pushed far beyond its normal (ward) limits.
I don't know who, or whether anybody has the right to decide when enough is enough. As doctors our patients and their relatives look to us for advice, and we give it as we can, albeit based on subjective judgements.
Post a Comment