"65 year old man, previously well. Single vehicle MCA, ejected through windscreen. 4-wheel drive versus tree in an 80 k zone." As the ambulance paramedic continues talking, an extra ED nurse starts filling in her clipboard. "Patient was unconscious at the scene with GCS 5 (tick) BP 90/60 (tick) Resp Rate 20 (tick), he was diaphoretic and shut down. Intubated at the scene with difficulty."
"Why say 'diaphoretic' when you can say 'sweaty'?" I think to myself. It annoys me as much as when people say 'pussy' instead of 'purulent'. I have dreams of infected abscesses exuding cats. Call me weird if you will.
As the ambo keeps talking, I start examining the patient. He is intubated, unconscious and paralysed. I can hear breath sounds throughout the lungfields and there's no dullness on percussion. There are some clinically fractured ribs on the right. "Good," I think, "No need for a chest tube here - yet." BP 100/60, Pulse rate 100, thankfully the fluids are going in through two nice big 16G IVs.
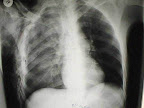 Primary survey over, I complete my secondary survey - forehead laceration with a small right occipital haematoma, cervical spine roughly in place (and patient asleep), clavicles and upper limbs intact, rib crepitus on the right, lax, paralysed abdomen, pelvis intact, and a left femoral shaft fracture. As I describe my findings for the benefit of our ED registrar, I see the nurse in the corner of my eye going "tick, tick, tick-tick". She seems strangely quiet as I check his urethra and do a PR. I'm much happier when I feel bounding pedal pulses. Chest and Cervical Spine X-rays show some early pulmonary contusion, no haemo- or pneumothorax and aforementioned rib fractures.
Primary survey over, I complete my secondary survey - forehead laceration with a small right occipital haematoma, cervical spine roughly in place (and patient asleep), clavicles and upper limbs intact, rib crepitus on the right, lax, paralysed abdomen, pelvis intact, and a left femoral shaft fracture. As I describe my findings for the benefit of our ED registrar, I see the nurse in the corner of my eye going "tick, tick, tick-tick". She seems strangely quiet as I check his urethra and do a PR. I'm much happier when I feel bounding pedal pulses. Chest and Cervical Spine X-rays show some early pulmonary contusion, no haemo- or pneumothorax and aforementioned rib fractures. The left leg goes into traction, and then off for a CT scan of his head (left parietal contre-coup contusion with a small subdural haematoma - "tick-tick"), neck (normal - but the collar stays on), and abdomen (minor hepatic laceration - "tick"). The femur gets nailed while the neurosurgeons put in an ICP monitor and the patient goes to ICU intubated with a Philadelphia collar until he wakes up.
The left leg goes into traction, and then off for a CT scan of his head (left parietal contre-coup contusion with a small subdural haematoma - "tick-tick"), neck (normal - but the collar stays on), and abdomen (minor hepatic laceration - "tick"). The femur gets nailed while the neurosurgeons put in an ICP monitor and the patient goes to ICU intubated with a Philadelphia collar until he wakes up.I'm left wondering what all that ticking is about - and then I realise... it is the scoring for the trauma audit. Our nurse is calculating the patient's probability of survival. And for my patient it is 27.6%. Do I care what it was? Would I have stopped, had I known his poor likelihood of survival? I don't think so. But it looks like a great business opportunity to me.
 That's why I am introducing the digital Probablility of Survival (pS) monitor. This little device will use advanced voice-recognition software as the registrar describes his findings, and with some fancy wireless networking, will pick up the observations from all other monitoring equipment. Using my secret modified algorithm a much more accurate probability of survival will be calculated every 5 seconds, so that you can know exactly when to stop resuscitation.
That's why I am introducing the digital Probablility of Survival (pS) monitor. This little device will use advanced voice-recognition software as the registrar describes his findings, and with some fancy wireless networking, will pick up the observations from all other monitoring equipment. Using my secret modified algorithm a much more accurate probability of survival will be calculated every 5 seconds, so that you can know exactly when to stop resuscitation.Imagine all the unnecessary exploratory laparotomies and ICU time that could be avoided. All the CTs and MRIs and IVC filters that wouldn't be wasted. We could resuscitate people until their pS fell below the economically viable threshold for the hospital. I don't believe in the device one little bit, but at US$1000 each, 5 for each ED worldwide, imagine the money I'd make!
I can't wait until my next invention is ready... the B-S monitor.





No comments:
Post a Comment